Ankylosis
Ankylosis is banded about willy-nilly, to avoid admission of failure and its possible legal consequences. This broader definition conveniently encompasses an array of errors of clinical judgement which include imprecise positional diagnosis, inappropriate directional traction, poorly designed or impotent biomechanics and inadequate anchorage preparation - after all, nobody can prove that the tooth was not truly ankylosed without doing the histology! Radiographs are singularly unreliable diagnostic aids in this respect and the use of CBCT in the determination of ankylosis has yet to be documented.
http://www.dr-adrianbecker.com/page.php?pageId=273
http://www.dr-adrianbecker.com/page.php?pageId=273
Ankylosis comes from Greek and means crooked, bent. When it comes to anatomy, it means that something is
stiff, stuck or fused together. More specifically in orthodontia it means fusion of mineralized root surface to the surrounding alveolar bone with the obliteration of the alveolar bone.
Causes are:
local metabolic genetic predisposition, dental trauma, luxation injuries, priapical infections, replantation of a
tooth after avulsion, chemical or thermal irritation, and previous surgical procedures. (1)
Diagnosis is mainly the inability of movement during orthodontic force applications, thus it can be either that
the tooth is truly stuck or that the orthodontist is incompetent (since the orthodontist is not going to say that he/she is incompetent, what you are going to hear is that the tooth is 'ankylosed...sorry...extraction'.)
Other old diagnostic tricks are 'metallic sounds upon percussion', failing the 'wiggle test' (when you luxate the
tooth it doesn't budge). Also radiologically maybe you can see 'an interruption of the periodontal membrane space on a radiograph'.(1)
Treatments are extraction and implant, surgical luxation, corticotomy, block osteotomy, auto transplantation, or, as described in the article (1), 'distraction osteogenesis'.
Surgical luxation would be to mild luxation of the tooth at surgery before attaching a bracket (4). This manoever
however, can also cause ankylosis it seems, why Dr. Puricelli is recommending apicoectomy in some cases (see
'dilaceration')
Dr Stella Chu writes about verifying whether or not the tooth is ankylosed first, before starting to treat it in her article on skeletal anchorage (5):
Case Report 1:...Before decidning on the retreatment plan, it was imperative to know wheather the canine
was ankylosed. A miniskrew was placed in the labial alveolar bone mesial to the first molar and a distally
directed force was applied to the canine. Lack of movement of the canine confirmed ankylosis. [the tooth
was extracted] A distinct bony bridge connecting the canine's labial aspect to the overlying alveolar bone was
observed at the time.
stiff, stuck or fused together. More specifically in orthodontia it means fusion of mineralized root surface to the surrounding alveolar bone with the obliteration of the alveolar bone.
Causes are:
local metabolic genetic predisposition, dental trauma, luxation injuries, priapical infections, replantation of a
tooth after avulsion, chemical or thermal irritation, and previous surgical procedures. (1)
Diagnosis is mainly the inability of movement during orthodontic force applications, thus it can be either that
the tooth is truly stuck or that the orthodontist is incompetent (since the orthodontist is not going to say that he/she is incompetent, what you are going to hear is that the tooth is 'ankylosed...sorry...extraction'.)
Other old diagnostic tricks are 'metallic sounds upon percussion', failing the 'wiggle test' (when you luxate the
tooth it doesn't budge). Also radiologically maybe you can see 'an interruption of the periodontal membrane space on a radiograph'.(1)
Treatments are extraction and implant, surgical luxation, corticotomy, block osteotomy, auto transplantation, or, as described in the article (1), 'distraction osteogenesis'.
Surgical luxation would be to mild luxation of the tooth at surgery before attaching a bracket (4). This manoever
however, can also cause ankylosis it seems, why Dr. Puricelli is recommending apicoectomy in some cases (see
'dilaceration')
Dr Stella Chu writes about verifying whether or not the tooth is ankylosed first, before starting to treat it in her article on skeletal anchorage (5):
Case Report 1:...Before decidning on the retreatment plan, it was imperative to know wheather the canine
was ankylosed. A miniskrew was placed in the labial alveolar bone mesial to the first molar and a distally
directed force was applied to the canine. Lack of movement of the canine confirmed ankylosis. [the tooth
was extracted] A distinct bony bridge connecting the canine's labial aspect to the overlying alveolar bone was
observed at the time.
Is the tooth stuck...or the orthodontist stuck?
The get-out-of-jail-free card: Just say it is 'ankylosed'
Another of my 'frustrated comments' gathered up:
In their July case report, “Attempted traction of impacted and ankylosed maxillary canines,” Oliveira and
Pithon report on their efforts to erupt impacted canines. But I wonder, did the attempt to erupt the canines
fail because they were ankylosed…or were the canines diagnosed as ankylosed after the attempt to erupt
them failed? The use of the term “ankylosed” in the article reflects a circular reasoning, ie, if traction placed
on the impacted canines does not erupt them, they must be ankylosed. In turn, if the canines are
ankylosed, they will not erupt. In my opinion, after 30 years of surgically exposing my cases with impacted
cuspids, very, very few are ankylosed. The most common operator error is insufficient removal of cortical
bone necessary to preclude a “pressure necrosis” between enamel of the erupting tooth and cortical bone
during a path of eruption. The physiologic process of bone resorption ahead of dental eruption has
terminated once the dental sac has been removed around the crown of an ankylosed tooth. Secondly,
traction needs to be continuous and renewed every 2 weeks. If eruption has not
occurred in 4 months, another exposure should be performed to remove scar tissue, expand the path of
eruption created through cortical bone, ascertain possible interference with adjacent roots, and, it is hoped,
leave the impacted tooth uncovered. With all due respect to the authors for submitting an interesting article
and achieving an excellent result, the “ankylosis” in the article did not exist. (2)
The author above, besides eloquently pointing out the dilemma of ego vs. presumed ankylosis, lays out a 'standard of practice' of how to handle impacted canines, that otherwise seems to be missing in orthodontics in the US:
expose and bond -> renew traction every 2 weeks -> if tooth doesn't move after 4 months -> renewed surgery
(hopefully CBCT sooner rather than later)
The whole processes done with the necessary imaging and consideration of what lies behind the tooth not moving carefully analyzed.
The dirty secret of orthodontics, all 'ankylosed' impactions are not ankylosed; or as it is put in a professional magazine talking of CBCT, the purported ankylosis might be a 'questional assumption' as below
James discussed some of the questionable assumptions we make with our typical orthodontic X-ray series:
If the tooth refuses to move it is ankylosed. He showed a case where the CBCT revealed a previously
undetected impaction that was blocking the stubborn tooth.(3)
In AJODO:
Invasive cervical root resorption is a lesion, which, in its early stages, is difficult to diagnose on a radiograph,
but, by the time the lesion has grown, bone is usually deposited in the depth of the resorption lacunae, and
the tooth will no longer respond to extrusive traction. It is our view that this is the cause of many failed
impacted teeth, rather than the knee-jerk and usually unproven application of the label "ankylosis".
Avoidance of extensive surgery down to the cementoenamel junction would appear to be called for, to
reduce the likelihood of the possible sequel.(6)
James discussed some of the questionable assumptions we make with our typical orthodontic X-ray series:
If the tooth refuses to move it is ankylosed. He showed a case where the CBCT revealed a previously
undetected impaction that was blocking the stubborn tooth.(3)
In AJODO:
Invasive cervical root resorption is a lesion, which, in its early stages, is difficult to diagnose on a radiograph,
but, by the time the lesion has grown, bone is usually deposited in the depth of the resorption lacunae, and
the tooth will no longer respond to extrusive traction. It is our view that this is the cause of many failed
impacted teeth, rather than the knee-jerk and usually unproven application of the label "ankylosis".
Avoidance of extensive surgery down to the cementoenamel junction would appear to be called for, to
reduce the likelihood of the possible sequel.(6)
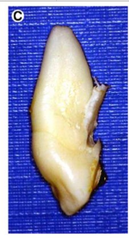
If extracted because of supposed ankylosis, the tooth needs to be studied and analysed microscopically afterwards to get the claim verified or not. I've only found one image of these 'ankylosed' teeth.
Also, 'ankylosis' is not a death-sentence for the tooth. Even if it is indeed partly fused to the alveolar bone it can be loosened ('coniotomy') or transplanted (see autotransplantation).
(1) Dolanmaz et al. Orthodontic Treatment of an Ankylosed Maxillary Central Incisor through Ostogenic
Distraction. The Angle Orthodontist. Volume 86, Issue 2, March, 2010.
(2) http://ajodoblog.blogspot.com/2012/07/letter-attempted-traction-of-impacted.html. American Journal of
Orthodontics and Dentofacial Orthopedics, July 31, 2012. Comment by DMD MSD Ron Parsons, Duluth, GA.
Commented on: http://www.ajodo.org/article/S0889-5406(12)00357-5/abstract
American Journal of Orthodontics & Dentofacial Orthopedics Volume 142, Issue 1 , Pages 106-114, July
2012, "Attempted traction of impacted and ankylosed maxillary canines" by Vinícius de Oliveira and
Matheus Melo Pithon Abstract: The aim of this article is to report the clinical orthodontic treatment of an
adult patient with 2 impacted maxillary canines. Traction was applied to the impacted teeth; however,
after 7 months, the teeth were found to be ankylosed and were extracted. The extraction spaces were
closed by moving the posterior teeth mesially with mini-implant anchorage. The results were satisfactory,
with the premolars in the functional position of the canines.
(3) The PCSO (Pacific Coast Society of Orthodontics Bulletin) winter 2008, 'The information Superhighway for
Orthodontists' reviews a presentation by Dr. James Mah at an orthodontist meeting.
(4) Seiler HF, Pajarola GF: Orale Chirurgie. In Farbatlanten derr Zahnmedicin, band. 11. Stuttgart: Georg
Thieme Verlag; 1996:71-140.
(5) Chaushu S, Chaushu G. Skeletal Implant Anchorage in the Treatment of Impacted Teeth -
A Review of the State of the Art. Seminars in Orthodontics, Vol 16, No 3 (September),
2010: pp 234-241.
(6) Becker A., Chaushu S. Palatally impacted American Journal of Orthodontic & Dentofacial Orthopedics.
Volume 143, Issue 4, p 451.)